There are many reasons why your baby may be unable to take all the milk they need directly from the breast. If your baby needs supplements (extra feeds) of expressed breastmilk or formula, you might like to consider using a nursing supplementer. This allows your baby to receive extra milk through a thin tube while feeding at the breast.
Using a supplementer can help you continue breastfeeding, even if feeding is not going as expected.
This article explains when a nursing supplementer might be useful, and how to use one.
Summary
- A nursing supplementer lets your baby receive extra milk at the breast, helping you continue breastfeeding.
- It can be useful if your baby needs supplements due to feeding difficulties, low milk supply, or other challenges.
- Using a supplementer can help support your milk production while your baby feeds.
- Supplementers can be used with expressed breastmilk or formula.
- With practice, many mothers and nursing parents find supplementers a helpful way to nurture their baby at the breast.
On this page
Why use a nursing supplementer?
A nursing supplementer can help you and your baby stay close while feeding, when extra milk is needed.
It may be helpful if your baby:
- Is not able to take enough milk directly from the breast
- Is slow to gain weight
- Is reluctant to latch or stay at the breast
It may also help if you:
- Are working to increase your milk supply
- Have a partial milk supply (for example, after breast surgery or with insufficient glandular tissue (IGT))
- Want to keep your baby feeding at the breast while giving supplements
Some families also use supplementers when:
- A baby has sucking or health difficulties 1
- A premature baby is learning to feed at the breast 2 3 4 5
- A non-birthing parent is breastfeeding (for example, adoptive or co- nursing) 6
Using a supplementer means your baby can receive extra milk while continuing to feed at the breast, building strength and skills to feed more effectively over time.
How it works
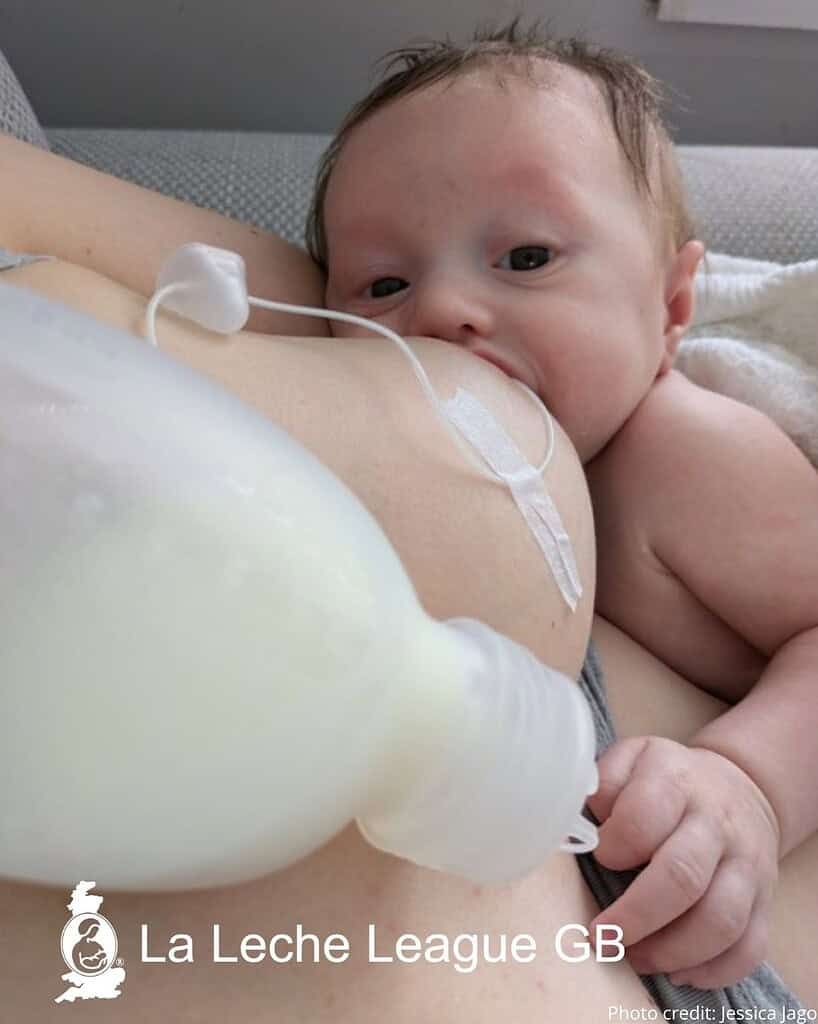
The supplementer holds the milk in a container. The milk travels through a thin tube into your baby’s mouth while they breastfeed. Your baby feeds as usual, while receiving extra milk through the tube.
A deep, comfortable latch is still important for your comfort, and so your baby can take as much milk as possible from the breast. However, even if your baby is not able to feed effectively from the breast, you can still use a supplementer and enjoy the closeness of breastfeeding.

Types of milk
Expressed breastmilk
Your own expressed breastmilk is the first choice. If your baby is having feeding difficulties, expressing protects your milk production.
Donor milk
Human milk banks provide screened, pasteurised donor milk, usually prioritised for premature or sick babies.
Informal ‘milk sharing’ – where surplus breastmilk is shared directly between families – has become more common in recent years. If you’re considering this, it’s important to follow safety guidance carefully.
Formula
Supplementers can also be used with formula.
Ready-to-feed infant formula is less likely to clog nursing supplementer tubing than powdered formula. It may also be more convenient when you are out or without support.
Always follow NHS safety guidelines when preparing formula.
You might use formula:
- As a temporary measure while increasing your milk production.
- Long-term, if you have a partial milk supply.
Whatever your situation, a supplementer allows you to continue feeding your baby at the breast.
Types of supplementer
Commercial supplementers
Come as complete systems, with different features:
- Bottle or bag systems
- Top or bottom openings
- Single or double tubes (useful for switching sides or feeding twins)
- Adjustable flow controls
- Different tubing sizes
Homemade supplementers
Some families choose to make their own supplementer using a bottle, teat, and infant feeding tube.
If you are considering this, it’s important to understand that these are not regulated feeding devices. Discuss your plans with a healthcare professional and follow appropriate hygiene guidance.
Basic setup includes:
- A bottle and teat
- A feeding tube threaded through the teat
- A small air hole or vent to allow milk flow
The bottle needs to stay upright. Some parents tuck it into their bra to keep it in place.
How to use a nursing supplementer
If you can, set up your supplementer in advance of a feed. Trying to put everything together when your baby is hungry and crying can feel stressful.
Placing the tube
You can experiment to find what works best.
- Position the tube alongside the nipple as your baby latches
- Place it along your baby’s tongue if they dislike it touching the palate
- Or slip it into the corner of your baby’s mouth once they are latched
- Adjust the length if needed
Fixing the tube
This isn’t essential, but can be helpful.
- Secure with medical tape (along the tube for a better hold)
- Some mothers use fabric plasters to reduce skin irritation and help reposition easily
Timing
- Start feeding at the breast first, then introduce the supplementer if swallowing slows
- Or begin with the supplementer if your baby is reluctant to latch
Speed
Your baby still needs to actively suck. Too fast a flow can reduce effective feeding.
You can adjust flow by:
- Changing the height of the container
- Using different tubing sizes – experiment to see what works best.
- Pinching or clamping the tube
Watch for signs your baby is overwhelmed, especially if they are premature or have health concerns.
Cleaning
Good hygiene is important.
• Follow manufacturer instructions for commercial systems
• For homemade systems, follow NHS guidance for bottles and teats
• Use a syringe to flush the tubing with cold water immediately after use
• Wash with hot soapy water, rinse well, and dry thoroughly
• Store clean parts in a sealed container in the fridge
Nasogastric tubes are not designed for repeated sterilisation. Replace them regularly (around weekly), or sooner if they stiffen.
If your baby has a higher risk of infection, a commercial system may be a safer option.
Getting started
Learning to use a supplementer can feel complicated at first. With practice, many mothers find it gets easier, and becomes an enjoyable way to feed their baby.
You don’t have to use it all the time. Some parents use supplementers only at certain times of day, or only at home – whatever works best for you and your baby.

Seek Support
If you are using a supplementer, whether short-term or longer-term, support can make a big difference.
An LLL Leader or group can offer practical suggestions and encouragement. You may also find it helpful to work with an IBCLC (lactation consultant) or specialist breastfeeding clinic.
When feeding isn’t going as you hoped, it can feel disappointing or overwhelming. A supplementer can be one way to keep your baby close at the breast, while making sure they are getting the milk they need.
Every feeding journey looks different. Finding a way that works for you and your baby – even if it’s not what you expected – is something to feel proud of.
You don’t have to work this out alone. Support is here for you.
Written by Karen Butler, Sue Upstone & mothers of LLLGB.
Updated by Cat Murray and Jayne Joyce, with thanks to Ellie Rowling, March 2026
Photos courtesy of Lynn Adams, Rae Vacher Lowe and Alison Widdup.
If this article has helped you, please consider supporting LLLGB with a donation. Every gift, however small, helps keep breastfeeding information and support flowing.
Further reading
Positioning and attachment
My Baby Needs More Milk
My Baby Won’t Breastfeed
Expressing and storing Your Milk
How to Increase Your Milk Supply
Using donor milk and formula to support breastfeeding
Relactation and Induced Lactation
Supplementer stories from LLLGB
In praise of at-breast supplementers
Breastfeeding with a nursing supplementer
Russell’s breastfeeding journey – breastfeeding a cleft-affected baby
La Leche League International
At-breast supplementer nursing
Other websites
Homemade Supplemental Nursing System, April 2025 (accessed 18 March 2026)
NHS leaflet: Guide to bottle feeding, 2022 (accessed 18 March 2026)
Books
The Art of Breastfeeding, 9th edition (La Leche League International, 2024), chapter 17.
Making More Milk Second Edition. Marasco, L and West, D., NY: McGraw-Hill, 2019.
Copyright LLLGB 2026.
References
- Haggarty Edwards, Moira et al. “Use of At-Breast Supplementers to Facilitate Feeding Solely at the Breast for Infants with Retrognathia: Two Case Studies.” Breastfeeding medicine : the official journal of the Academy of Breastfeeding Medicine vol. 19,3 (2024): 228-231. doi:10.1089/bfm.2023.0268 https://www.liebertpub.com/doi/10.1089/bfm.2023.0268 (Accessed 18 March 2026) ↩︎
- Noble, Lawrence M et al. “ABM Clinical Protocol #12: Transitioning the Breastfeeding Preterm Infant from the Neonatal Intensive Care Unit to Home, Revised 2018.” Breastfeeding medicine : the official journal of the Academy of Breastfeeding Medicine vol. 13,4 (2018): 230-236. doi:10.1089/bfm.2018.29090.ljn ABM Clinical Protocol #12: Transitioning the Breastfeeding Preterm Infant from the Neonatal Intensive Care Unit to Home, Revised 2018 (Accessed 18 March 2026) ↩︎
- Gülbetekin, Eda, and Fatma Gül Can. “The Effect of Supplemental Nursing System on Sucking Success, Weight Gain Findings and Bilirubin Level in Newborns: A Randomized Controlled Trial.” Maternal and child health journal vol. 29,2 (2025): 258-268. doi:10.1007/s10995-025-04039-0 https://journals.sagepub.com/doi/10.1177/10547738211058312?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%20%200pubmed (Accessed 18 March 2026) ↩︎
- Çelik, Fikriye et al. “Effects of Oral Stimulation and Supplemental Nursing System on the Transition Time to Full Breast of Mother and Sucking Success in Preterm Infants: A Randomized Controlled Trial.” Clinical nursing research vol. 31,5 (2022): 891-900. doi:10.1177/10547738211058312 https://journals.sagepub.com/doi/10.1177/10547738211058312 (Accessed 18 March 2026) ↩︎
- Gozen, Duygu et al. “Effect of the Supplemental Nursing System on the Oral Feeding Skills of Preterm Infants: A Randomized Controlled Study.” American journal of speech-language pathology vol. 34,6 (2025): 3389-3399. doi:10.1044/2025_AJSLP-25-00027 https://pubs.asha.org/doi/10.1044/2025_AJSLP-25-00027?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%20%200pubmed (Accessed 18 March 2026) ↩︎
- Cheales-Siebenaler, N J. “Induced lactation in an adoptive mother.” Journal of human lactation : official journal of International Lactation Consultant Association vol. 15,1 (1999): 41-3. doi:10.1177/089033449901500111 https://journals.sagepub.com/doi/10.1177/089033449901500111?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%20%200pubmed (Accessed 18 March 2026) ↩︎
